Introduction
Since the 1970s, platelet-rich plasma (PRP) therapy has grown in popularity, with current applications spanning a wide range of specialties, from orthodontics and orthopedics to cosmetics, among others. The regenerative technique uses a high concentration of a patient’s own blood platelets to stimulate healing in damaged tissue, rejuvenate skin, regrow hair, and more.
As research mounts indicating the method can be used to treat various conditions and illnesses, PRP therapy is more and more becoming the way of the future. Some studies have even indicated PRP could potentially be an improved alternative to surgeries.
Hyperbaric Medical Solutions (HMS) created this guide to help readers understand what platelet-rich plasma is, how PRP therapy works and its roots, explore the conditions it can treat, and how PRP and HBOT combine to create a powerful healing accelerant.
CHAPTER 1
Defining Platelet-Rich Plasma
Before defining platelet-rich plasma, it’s important to understand what platelets and plasma are, and their importance to the body.
Platelets, also called thrombocytes, are disk-shaped blood cells that circulate throughout the body and help form blood clots to stop bleeding. A natural source of growth factors, platelets contain platelet-derived growth factor (PDGF), insulin-like growth factor (IGF), vascular endothelial growth factor (VEGF), platelet-derived angiogenic factor (PDAF), and transforming growth factor beta (TGF-β). These are released when platelets are activated. .
Platelets also release other substances important to healing, such as fibronectin (plays a role in adhesion, migration and growth), vitronectin (cell adhesion and spreading factor), sphingosine 1-phosphate (angiogenesis and immune responses).Plasma is the medium through which platelets and red and white blood cells move. The liquid portion of blood, it is generally composed of water and proteins. Plasma and high concentration of platelets are referred to as platelet rich plasma (PRP).
CHAPTER 2
What Is PRP Therapy?
Platelet-rich therapy utilizes injections to harness the power of PRP and support regeneration. Let’s run through how platelet-rich therapy is administered, the recovery process, and any side effects there may be.
Procedure
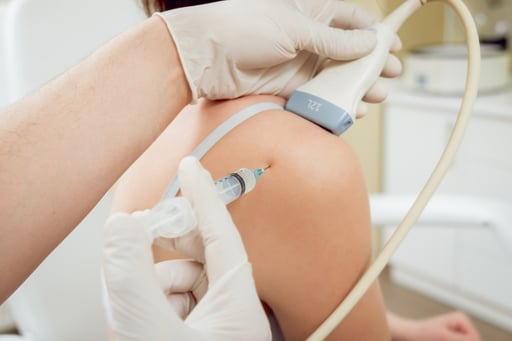
To start the procedure, blood is drawn from the patient like any other ordinary blood draw. The sample is then placed in a special centrifuge, which is used to separate the blood into layers. Within minutes, the PRP portion of the blood, containing platelets, cytokines and growth factors is extracted into a syringe for injection at the point of injury, or area of the body being attended to. The separated PRP portion of the blood consists of more platelets than regular blood.
This platelet-rich plasma is then injected directly into the wounded or diseased body tissue, releasing growth factors and stimulating the production of reparative cells. Ultrasound imaging is used to ensure its precise placement in the tissue. The entire process takes about 30 minutes.
The number of injections of PRP will depend on the condition or desired outcome.
Recovery
Recovery from PRP therapy entails minimal downtime. Improvement varies by patient depending on severity of their condition and results occur anywhere from several weeks to a few months after treatment.
Side Effects
Because the PRP concentration is made from a patient’s own blood, there’s no risk of allergic reaction or transmission of a communicable disease in connection with the use of your own blood. Possible side effects include mild pain or tenderness at the injection site, swelling, temporary bleeding or injury to tissue.
CHAPTER 3
History of Platelet-Rich Plasma Therapy
Researchers discovered the regenerative potential of platelets in the 1970s. One study observed platelets “clearly play a complex role in stimulating the response of tissues to injury” and are responsible for increased collagen production, cell mitosis, blood vessel growth, migration to the site of injury, and more.
During that time, the term PRP wasn’t yet thought of as a means to heal injuries directly, however. PRP was used as a treatment for thrombocytopenia, a condition characterized by a low blood platelet count.
Several years later, physicians began using PRP for maxillofacial surgery, periodontal surgery, and cosmetic surgery to cut down on blood loss during operations. In the early 2000s, PRP expanded into orthopedics, proving to boost healing in fractures and bone grafts.
As research continued and trials proved successful, PRP became a common procedure to treat connective tissue repair in sports medicine. In 2006, the first human study “Treatment of Chronic Elbow Tendinosis with Buffered Platelet-Rich Plasma” was published in The American Journal of Sports Medicine, reporting an immediate 60-percent improvement, an 81-percent improvement at six months, and a 93-percent decrease in pain after two years.
PRP skyrocketed to popularity when professional golfer Tiger Woods admitted to undergoing PRP therapy just before his comeback in 2010. At the time, the public didn’t know much about the regenerative procedure. Soon after, articles explaining PRP and how it works flooded the internet, as more and more athletes announced they, too, underwent the treatment. This included the late Kobe Bryant (arthritic right knee), Golden State Warriors star Stephen Curry (Grade 1 MCL sprain in his right knee), San Diego Padres pitcher Garrett Richards (torn elbow ligament), and Detroit Piston Reggie Jackson (tendinosis and ulnar collateral ligament sprain in his thumb). The list has only grown as more and more professional and collegiate sports teams use PRP with higher frequency to treat an array of injuries. While gaining popularity in sports, others experiencing a range of injuries from knee arthritis to fractures can utilize PRP to heal.
In 2019, researchers conducted a systematic review of 132 papers and 11 articles on PRP as a treatment for hair loss. The study concluded: “Most studies suggest that subcutaneous injection of PRP is likely to reduce hair loss, increase hair diameter and density in patients with androgenic alopecia.”
Now, PRP therapy is used in a number of cosmetic and aesthetic procedures to restore a youthful appearance.
CHAPTER 4
What Conditions Can PRP Treat?
PRP can be used for a variety of musculoskeletal repairs, aesthetic improvements for skin and hair and enhanced sexual health. The uses of PRP include:
Osteoarthritis
Osteoarthritis, which affects more than 30 million adults in America, has proven to be treatable with PRP therapy. A systematic review titled “Platelet-rich Plasma in Osteoarthritis Treatment: Review of Current Evidence” published in the journal Therapeutic Advances in Chronic Disease concluded “results from randomized clinical trials seem to favor PRP used over other intra articular treatments such as HA injections, to improve pain scales in the short and medium term (6–12 months).” Because Osteoarthritis is most commonly found in the knee, multiple studies have been conducted to understand PRP’s effect on this joint. One study found “Intra-articular PRP injections into the knee for symptomatic early stages of OA are a valid treatment option. The clinical efficacy of IA-PRP is comparable to that of the IA-HA and IA-CS forms after 3 months and the long-term efficacy of IA-PRP is superior to IA-HA and IA-CS.”
Tendon Injuries & Rotator Cuff Tendinopathy
Orthopedic specialists and sports medicine physicians have been using PRP injections to treat patellar, quadriceps, hamstring, bicipital, peroneal, and achilles injuries. Researchers conducted a systematic review of multiple studies and concluded multiple beneficial effects of PRP, including pain reduction, joint function improvement and tissue repair.”
Also an effective treatment for rotator cuff tendinopathy, PRP “resulted in sustained improvement of pain, function, and MRI outcomes in patients,” states another study.
Bursitis
Researchers have found evidence PRP can be used to treat bursitis, a painful condition affecting the bursae that cushion bones, tendons, and muscles near joints, and greater trochanteric bursitis, inflammation of the bursa at the outside point of the hip. One study discovered PRP injections more effective than cortisone for chronic hip bursitis.
Medial & Lateral Epicondylitis
Studies have shown patients with these conditions, also known as golfer’s (medial) and tennis (lateral) elbow, have experienced pain reduction and increased function after PRP injection. One study concludes PRP therapy exhibits greater improvement than a cortisone injection.
.jpeg)
Aesthetic Use
In more recent years, PRP has been used for such aesthetic purposes as facials. One study found PRP injections rejuvenated the skin in the lower eye region, while another discovered PRP promotes “tissue remodeling in aged skin and may be used as adjuvant treatment to lasers.”
A “reverse aging” result can be found using PRP therapy by restoring layers of collagen, reducing fine lines, wrinkles, stretch marks, and scarring, and a tightening of the skin.
Hair Loss
Many studies have demonstrated PRP as an effective treatment for androgenic alopecia, a common hair disorder affecting 45 percent of men and 35 percent of women over the age of 60. Most showed evidence of hair regrowth after three months.
Sexual Health
The principles of PRP therapy can also be used to enhance sexual function or treat sexual disorders. The restoration of blood supply can enhance sensation and have lasting effects for erectile dysfunction in males and for vaginal rejuvenation in females.
Other treatable conditions include plantar fasciitis, ulnar collateral ligament sprain or tear, ankle sprain or ligament injury, hamstring tears, knee pain, muscle injuries, ligament sprains or tears (MCL, LCL), hip pain, lower leg and foot pain, shoulder and arm pain, shin splints, and Achilles tears.
CHAPTER 5
Combining PRP & HBOT
While it is not often thought of this way, hyperbaric oxygen therapy (HBOT) is also a regenerative medicine technique, and individually, both PRP therapy and HBOT can accelerate recovery. However, combining PRP therapy and HBOT has powerful stimulating and healing effects—enabling patients to achieve more optimal results and even avoid long and burdensome surgeries.
Platelets act as magnets for stem-cells, and HBOT is proven to release and mobilize stem-cells from the bone marrow, increasing circulation above normal by up to 8x. By utilizing HBOT before and after each PRP injection, the injected PRP attracts these STEM CELLS to the area in need to promote accelerated healing.
The combination can also ease any aches or soreness that may result from PRP therapy alone. Our combined approach has been very sucessful when treating knee pain, tendon injuries, ligament sprains or tears, bursitis, hip pain, osteoarthritis, tendonitis, shin splints, medial and lateral epicondylitis, hamstring injuries, diabetic wounds, and more.
PRP and HBOT aren’t just for healing conditions. They can have aesthetic and rejuvenating impacts on skin, hair, and sexual health. Known as a reverse aging technique, PRP and HBOT can reveal a youthful glow, restore layers of collagen, reduce fine lines, wrinkles, stretch marks, and acne scars. The combo can grow and thicken hair without surgery. Plus, it has the ability to enhance sexual function. For males, the two modalities can restore blood supply, repair sensation, and help with Erectile Dysfunction. For females, it enhances sensation and provides vaginal rejuvenation.
Hyperbaric Medical Solutions can design a specialized program to deliver regenerative medicine techniques such as HBOT and PRP to support tissue repair, restore health, optimize healing, and enhance functions. Each plan is based on the individualized needs of the patient, and every program begins with a comprehensive consultation and evaluation with Dr Alan Katz, our Medical Director who is double board certified in emergency medicine and hyperbaric medicine.
